Crohn’s disease — or Maladie de Crohn as it is known in French — can feel like an unwelcome roommate that shows up without warning and refuses to leave. If you or someone you love has been diagnosed, you’ve probably already noticed how it changes the rhythm of daily life: unpredictable symptoms, complicated medical decisions, and a steady stream of questions about food, work, and the future. This article aims to be a practical, compassionate companion. I’ll walk you through what Crohn’s disease is, how it’s diagnosed, the wide range of treatment options, and the emotional and lifestyle strategies that make life livable and meaningful despite the disease.
You don’t need to become a medical expert to manage Crohn’s, but knowledge helps you make better choices and feel more in control. I’ll explain medical concepts in clear language, give actionable tips for day-to-day living, and include honest talk about uncertainty. Whether you’re newly diagnosed, supporting someone, or living with Crohn’s for years, this piece is written to help you understand triggers, treatments, and how to thrive — not just survive.
What is Crohn’s Disease?
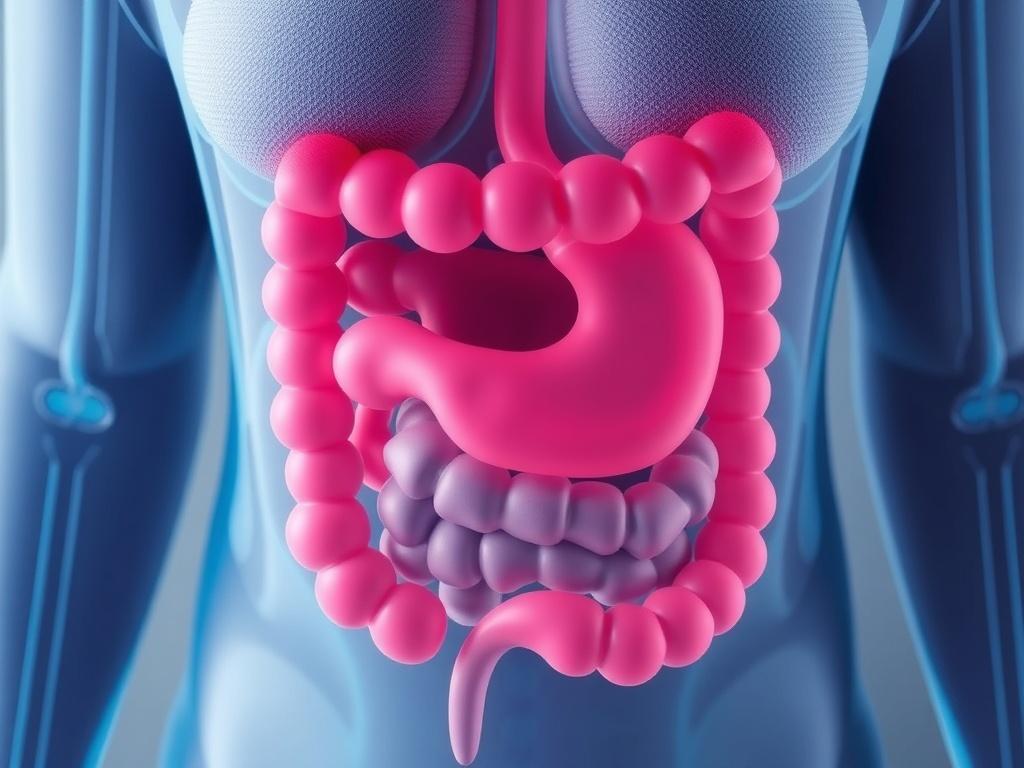
Crohn’s disease is a type of inflammatory bowel disease (IBD) that causes chronic inflammation of the digestive tract. Unlike ulcerative colitis, which affects only the colon and rectum, Crohn’s can affect any part from the mouth to the anus. In most people it targets the end of the small intestine (the ileum) and the beginning of the colon, but the pattern varies widely. The inflammation can be patchy, affecting some segments while leaving others entirely normal.
This inflammation can penetrate deeply into the layers of the intestinal wall, causing symptoms like abdominal pain, diarrhea, fatigue, weight loss, and sometimes fever. Over time, ongoing inflammation may lead to complications such as strictures (narrowed segments), fistulas (abnormal connections between organs), abscesses, and nutrient deficiencies. Crohn’s is considered an immune-mediated disease, which means the immune system plays a central role, though genetics, environment, and the gut microbiome are also part of the story.
Who gets Crohn’s disease?
Crohn’s can begin at any age but most commonly appears between ages 15 and 35. It affects men and women roughly equally and occurs worldwide. Genetics matter: having a family member with Crohn’s increases risk, but most people with Crohn’s do not have a close family member with it. Environmental factors — such as smoking, diet, and perhaps antibiotic use in early life — have been associated with higher risk or more severe disease.
Importantly, Crohn’s is not caused by stress or poor parenting. Stress can trigger flares in someone who already has Crohn’s, but it isn’t the root cause. Understanding risk factors helps but does not change the day-to-day management that keeps people well.
How Crohn’s Disease is Diagnosed
Diagnosing Crohn’s disease typically requires a combination of medical history, blood tests, stool tests, imaging, and endoscopy with biopsy. There is no single “Crohn’s test,” so clinicians look for a pattern of evidence.
Blood tests may show signs of inflammation (such as an elevated C-reactive protein, CRP) or anemia. Stool calprotectin is a useful noninvasive marker that indicates intestinal inflammation and helps distinguish inflammatory conditions from irritable bowel syndrome (IBS). Endoscopy (colonoscopy or upper endoscopy) allows direct visualization and biopsy of the gut lining; pathology showing granulomatous inflammation can point to Crohn’s, although it’s not present in every case.
Imaging tests like MR enterography or CT enterography visualize the small bowel and detect complications like strictures or fistulas. Capsule endoscopy, where a tiny camera is swallowed, can inspect parts of the small intestine not easily reached by standard endoscopy. The diagnostic journey can be frustrating because symptoms overlap with other conditions, infections can mimic Crohn’s, and initial tests may be normal.
Key diagnostic steps
- Detailed medical history and physical exam
- Blood tests: CBC, CRP, ESR, nutrients (iron, B12, vitamin D)
- Stool tests: calprotectin, stool cultures if infection suspected
- Colonoscopy with biopsies
- Cross-sectional imaging: MR or CT enterography
- Small bowel evaluation: capsule endoscopy when appropriate
Symptoms and Complications: What to Watch For
Symptoms range from mild and intermittent to severe and persistent. Some days you may feel nearly normal; other days you may be struggling with pain and fatigue. Common symptoms include:
- Chronic or recurrent abdominal pain
- Diarrhea, sometimes with blood or mucus
- Urgency and incontinence during flares
- Weight loss and poor appetite
- Fatigue and general malaise
- Fever during active inflammation
- Perianal pain, fissures, fistulas, or drainage
Complications can be serious and may require surgical or advanced medical treatment:
- Intestinal strictures causing bowel obstruction
- Fistulas connecting bowel to bladder, skin, or other loops
- Abscesses requiring drainage
- Nutrient deficiencies such as iron, B12, vitamin D
- Increased risk of some cancers in long-standing disease (surveillance is important)
The unpredictability of symptoms can make planning ahead hard, but many people learn how to manage flares and maintain stable periods for months or years.
Red flags — when to seek urgent care
- Severe abdominal pain or signs of bowel obstruction (vomiting, severe distension)
- High fever not controlled by antipyretics
- Heavy bleeding that causes faintness or rapid heart rate
- Signs of sepsis: confusion, very low blood pressure
- Severe dehydration from diarrhea
If you experience any of these, seek emergency medical care.
Treatments: Medical, Nutritional, and Surgical Options
The treatment goal in Crohn’s disease is to control inflammation, relieve symptoms, heal the intestinal lining, prevent complications, and maintain quality of life. Treatment is tailored to disease location, severity, pattern (inflammatory, stricturing, or penetrating), and patient preferences.
Medical therapies
Medical options have expanded significantly over the past decades and now include anti-inflammatory drugs, immunomodulators, biologic therapies, and small-molecule drugs. Treatment often begins with less aggressive options and escalates if needed.
- Aminosalicylates (5-ASA): Historically used for mild disease, more helpful in ulcerative colitis than Crohn’s.
- Corticosteroids: Effective to induce remission quickly but not for long-term use due to side effects like osteoporosis, weight gain, and infection risk.
- Immunomodulators: Azathioprine, 6-mercaptopurine, and methotrexate can maintain remission and reduce steroid dependence. They require regular blood monitoring.
- Biologics: Anti-TNF agents (infliximab, adalimumab), anti-integrin (vedolizumab), anti-IL12/23 (ustekinumab) target specific immune pathways and can be very effective, especially for moderate to severe disease.
- Small molecules: Janus kinase (JAK) inhibitors and other oral agents are now available for some patients and offer another route when injections or infusions are not ideal.
Monitoring and side effects
With immunosuppressive treatments, careful monitoring is essential: blood counts, liver tests, TB screening before anti-TNF therapy, and vaccinations up to date. Side effects range from mild (headache, injection site reactions) to serious (infections, rare malignancies). Discuss risks and benefits openly with your provider; for many patients, the benefits of controlling inflammation outweigh the risks.
Nutritional strategies
Nutrition is a central concern. Crohn’s can impair nutrient absorption due to inflammation, surgery, or reduced intake. Work with a dietitian experienced in IBD when possible. Important nutritional strategies include:
- Correcting deficiencies: iron, B12, vitamin D, calcium, and others as needed.
- Using exclusive enteral nutrition (a liquid diet) as induction therapy in some cases, especially in children.
- Short-term low-residue diets during flares to reduce bowel volume and pain.
- Small, frequent meals and attention to hydration.
- Identifying and avoiding personal trigger foods, not necessarily following one-size-fits-all diet plans.
Many people find keeping a food-and-symptom diary helps uncover patterns. Avoid drastic dietary restrictions without medical guidance; eliminating multiple food groups can create nutritional problems.
Surgery — when and why
Despite advanced medical therapies, many people with Crohn’s will require surgery at some point to treat complications like strictures, fistulas, or abscesses. Surgery is not a cure because Crohn’s can recur in other parts of the intestine, but it can resolve immediate problems and improve quality of life. Surgeons now use more conservative approaches when possible to preserve bowel length.
After surgery, medical therapy often continues to reduce the risk of recurrence. Coordination between gastroenterologists, surgeons, and patients helps choose the right timing and approach.
Living with Crohn’s: Practical Tips for Daily Life
Managing Crohn’s is more than taking medication — it involves sleep, stress management, relationships, work, and planning around unpredictability. Here are practical tips gathered from patients, clinicians, and everyday experience.
Symptom planning and flare management
Have a plan for flares that includes who to call, medication adjustments (under medical advice), and steps to take for hydration and nutrition. Keep a small emergency kit with:
- Prescription medications and a copy of current treatment plan
- Oral rehydration salts or electrolyte drinks
- Portable heating pad for abdominal cramping
- A list of medical contacts and recent lab results
Learning early signs of a flare (increased bowel movements, worsening pain, rising fatigue, or elevated CRP) can prompt faster treatment and prevent complications.
Work, education, and social life
Many people with Crohn’s work full-time, study, and maintain rich social lives. Open communication with employers and educators can help obtain necessary accommodations, like flexible schedules or restroom access. Consider these strategies:
- Request reasonable accommodations under workplace disability laws if needed.
- Use telecommuting during flares when possible.
- Plan social events with knowledge of nearest restrooms and dietary options.
- Carry a “flare card” that succinctly explains your condition for urgent situations.
Managing energy levels is important; fatigue is real and must be respected. Prioritize tasks and avoid overbooking during unpredictable periods.
Travel tips
Travel can be anxiety-provoking but is entirely possible with preparation. Pack extra medication, copies of prescriptions, a doctor’s letter for airport security if needed, and a list of local medical centers at your destination. Pack easy-to-digest snacks and consider travel insurance that covers medical needs.
Mental Health and Coping: The Invisible Side of Crohn’s
Living with a chronic illness like Crohn’s affects mental health. Anxiety about flares, body image issues from weight changes or surgical scars, and the social isolation of frequent bathroom use are very real. Addressing mental health is as important as treating physical symptoms.
Common emotional responses
- Grief and frustration over loss of predictable health
- Fear of complications or needing surgery
- Anxiety about flares and social embarrassment
- Depression in some people, especially during prolonged active disease
Therapy, support groups, and peer networks can be tremendously helpful. Cognitive-behavioral therapy (CBT), mindfulness, and acceptance-based strategies can reduce anxiety and improve coping. Many IBD centers offer integrated care with mental health professionals.
Practical coping strategies
- Build a support network: friends, family, online communities, and support groups.
- Set realistic goals and celebrate small victories during remission.
- Practice stress-reduction: brief daily breathing exercises, walking, or yoga tailored to energy levels.
- Consider professional help early when mood or anxiety become persistent.
Remember that seeking support is a strength, not a sign of weakness.
Self-Advocacy: How to Work with Your Medical Team
You are the expert in how your body feels. Successful long-term care depends on a collaborative relationship with your gastroenterologist, nurse, dietitian, and possibly a surgeon or psychologist. Prepare for appointments with focused questions and clear priorities.
Questions to ask your doctor
- What is the likely pattern and location of my disease?
- What are the treatment goals: symptom control or deep remission with mucosal healing?
- What are the pros and cons of each medication option for me?
- How will we monitor my response to therapy (blood tests, imaging, colonoscopy)?
- What vaccinations or infection screening do I need before starting immunosuppressive therapy?
Keep a health journal with lab results, medication changes, and symptom trends — it helps detect patterns and supports better decisions.
Medications at a Glance: A Simple Table
Below is a simplified table comparing common medication classes, typical uses, and key side effects. This is a high-level summary; each medication has nuances and individualized considerations.
| Medication Class | Typical Use | How It Works | Key Side Effects / Considerations |
|---|---|---|---|
| Aminosalicylates (5-ASA) | Mild colon inflammation | Topical anti-inflammatory in gut lining | Kidney monitoring in some drugs; limited benefit in Crohn’s overall |
| Corticosteroids (prednisone) | Induce remission quickly | Suppress broad immune response | Weight gain, bone loss, infections; not for long-term use |
| Immunomodulators (azathioprine) | Maintain remission | Slows immune cell proliferation | Bone marrow suppression, liver tests; requires blood monitoring |
| Anti-TNF biologics (infliximab) | Moderate to severe disease, fistulas | Blocks TNF-alpha, a key inflammatory messenger | Infection risk (TB screening needed), infusion or injection therapy |
| Anti-integrin (vedolizumab) | Moderate to severe disease | Blocks gut-specific immune cell trafficking | Lower systemic infection risk; infusion therapy |
| Anti-IL12/23 (ustekinumab) | Moderate to severe disease | Targets interleukin signaling in immune response | Injection/infusion; infection monitoring |
| Small molecules (JAK inhibitors) | Moderate to severe disease when other therapies fail | Oral pills that modulate intracellular signaling | Blood clots risk in some patients; regular monitoring |
Diet and Nutrition: What the Evidence Says
Dietary advice is often confusing because scientific evidence is still evolving and individual responses vary. There is no single “Crohn’s diet” that works for everyone. However, there are evidence-based strategies and pragmatic tips.
Foods commonly reported to trigger symptoms
- High-fiber foods during flares (raw vegetables, whole nuts, seeds)
- Dairy if lactose intolerant
- Spicy foods in some people
- High-fat or fried foods that may worsen diarrhea
- Caffeine and alcohol can irritate the gut in some individuals
During remission, many people can resume a varied diet. In children, exclusive enteral nutrition is a proven treatment to induce remission and promote growth without steroids. In adults, enteral nutrition can help but is less commonly used outside pediatric settings.
Supplements and practical tips
- Check vitamin D and replace if low — deficiency is common.
- Monitor iron and B12; oral or IV supplementation may be needed.
- Probiotics have modest evidence in ulcerative colitis; benefits in Crohn’s are less clear but often tried.
- Work with a dietitian to avoid unnecessary elimination diets that risk malnutrition.
Small changes, personalization, and professional guidance are the keys to safe and effective dietary management.
Pregnancy, Fertility, and Family Planning
Many people with Crohn’s have healthy pregnancies, but planning is important. Active disease at conception or during pregnancy increases the risk of complications such as preterm birth or low birth weight. Therefore, the general recommendation is to achieve remission before conception.
Medication considerations
Many Crohn’s medications are safe in pregnancy; for example, some anti-TNF agents and certain immunomodulators have acceptable safety profiles, while methotrexate is contraindicated and must be stopped months before conception. Discuss medications with your gastroenterologist and obstetrician who specialize in high-risk pregnancies if needed. Breastfeeding is often possible, but medication choices may affect decisions.
Fertility
Fertility is usually normal for people with Crohn’s who are in remission. Active disease and some pelvic surgeries can affect fertility, so discuss options with your care team if you plan to conceive.
Children and Adolescents with Crohn’s
When Crohn’s begins in childhood, it brings special challenges: growth delay, school impact, and the emotional burden of dealing with a chronic condition during development. Pediatric gastroenterologists often use nutritional therapy more frequently, and growth monitoring is a high priority. Families benefit from comprehensive care teams including pediatric dietitians, psychologists, and transition planning as the child approaches adulthood.
Research, New Treatments, and Hope for the Future
Research in Crohn’s disease is active and encouraging. Advances in biologics and small molecules have created more options for personalized care. Studies of the gut microbiome, fecal microbiota transplantation, and novel therapeutic targets are ongoing. Predictive markers that forecast which drug will work best for which patient are under investigation, which could one day replace current trial-and-error approaches.
Clinical trials remain an important option for some people, particularly when standard therapies fail. Ask your care team about trials that might be appropriate; participation may provide access to cutting-edge treatments and contribute to broader scientific progress.
Common Myths and Misconceptions
Addressing myths helps reduce stigma and confusion. Let’s correct some common misunderstandings:
- Myth: Crohn’s is caused by stress. Reality: Stress can exacerbate symptoms but is not the primary cause.
- Myth: Surgery cures Crohn’s. Reality: Surgery treats complications but does not cure the underlying disease.
- Myth: You must starve yourself or follow extreme diets to stay healthy. Reality: Balanced, personalized nutrition is the goal — not unnecessary restriction.
- Myth: You can’t have children with Crohn’s. Reality: Many people with Crohn’s have healthy pregnancies with proper planning.
Clearing up misinformation empowers better self-care and reduces unnecessary fear.
Support Networks, Advocacy, and Practical Resources
Living with Crohn’s is easier when you’re not alone. Support groups — local or online — provide empathy, practical tips, and shared experiences. National and international organizations offer resources on patient rights, research, and educational materials. Mental health professionals and social workers can help with coping and navigating systems like disability and insurance.
Suggested practical resources
- Local IBD support groups or hospital-based patient education programs
- National organizations for patient education and advocacy
- Online forums and moderated communities for practical tips and emotional support
- IBD nurses and multidisciplinary clinics for coordinated care
When choosing online resources, prioritize reputable medical organizations, academic centers, and peer-reviewed content.
When to Consider a Second Opinion

A second opinion can be reassuring and sometimes essential when facing major decisions like starting a new biologic, contemplating surgery, or if symptoms are not responding to standard therapies. A fresh perspective can re-evaluate diagnosis, suggest alternative treatments, or recommend specialized care such as a multidisciplinary IBD clinic.
How to get a helpful second opinion
- Bring imaging, endoscopy reports, and pathology slides if possible.
- Ask specific questions: “Is there another treatment that could avoid surgery?”
- Use second opinions to inform rather than to delay necessary care.
Seek a balance between gathering information and acting decisively when urgent issues arise.
Practical Checklist: Living Well with Crohn’s
Here is a compact checklist you can use as a starting point to organize medical care and daily life.
- Keep a current medication list and emergency contact info in your wallet.
- Track symptoms and triggers in a journal or app.
- Schedule routine monitoring tests: bloodwork, bowel imaging as recommended.
- Keep vaccinations up to date before starting immunosuppressants.
- Build a support team: physician, nurse, dietitian, mental health provider.
- Plan for flares with an emergency kit and easy meals.
- Discuss fertility and pregnancy plans with your care team if relevant.
Small habits compound into resilient health management over time.
Final Thoughts

Crohn’s disease reshapes life in ways that are both practical and emotional. It’s a condition with ups and downs, but modern medical care, nutrition strategies, psychological support, and self-advocacy tools make long, fulfilling lives entirely possible. The journey involves learning about your personal disease pattern, partnering with clinicians, and building networks of support. While uncertainty is part of the experience, so is hope: new treatments continue to emerge, and many people with Crohn’s lead active, satisfying lives.
Conclusion
Living with Maladie de Crohn means navigating a complex condition that affects body and mind, but with accurate information, a supportive care team, thoughtful lifestyle adjustments, and emotional resilience you can manage flares, reduce complications, and maintain a high quality of life; prioritize regular medical follow-up, personalized treatment plans, good nutrition, mental health care, and practical preparations for work and travel, and remember that asking for support and seeking second opinions when needed are signs of strength that help you take control of your health and future.
Читайте далее: